Electronic Fetal Monitoring — No Benefits, Plenty of Harm
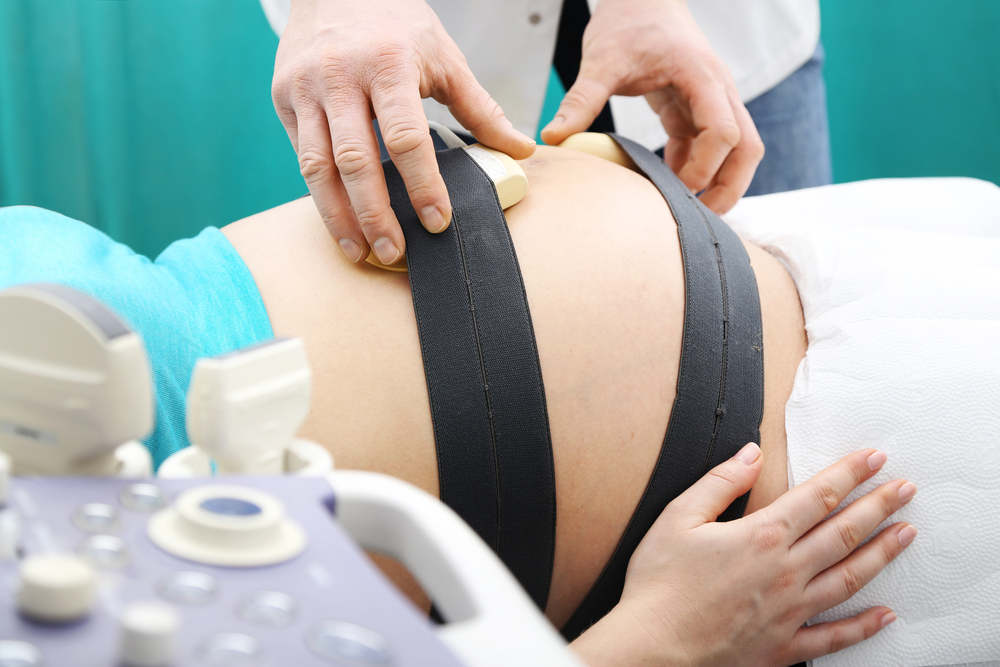
The increase in cesarean sections brought on by the use of electronic fetal monitoring during delivery has not reduced rates of cerebral palsy, instead placing women at high risk of complications and death.
The trend in using electronic monitoring, opting for cesarean sections at the slightest sign of abnormality, has been worsened by the risk of lawsuits that doctors face when delivering children vaginally who later turn out to have cerebral palsy.
In an analysis, titled “Electronic fetal monitoring, cerebral palsy, and caesarean section: assumptions versus evidence,” published in the journal The BMJ, researchers at the National Institute of Neurological Disorders and Stroke argue that it is time to change this practice.
When electronic fetal monitoring was introduced in the 1970s, people had high hopes that this would reduce the rates of cerebral palsy. At the time, scientists believed that the condition was caused by a lack of oxygen during delivery.
Today, cerebral palsy rates are at the same level, and studies show that using abnormal patterns in electronic monitoring to predict cerebral palsy fails in 99.8 percent of cases. Other birth complications, including death or the need for special newborn care, were also not prevented by the introduction of electronic monitoring, compared to manually repeated heart rate checks.
Obstetric societies in the U.S., Canada, Australia, and New Zealand have taken this information to heart and acknowledge that electronic monitoring does not provide any benefits in health outcomes for children.
So how can the use of electronic monitoring fail to be better than occasional checks of the fetus’s heart rate?
Studies have shown that decreases in the heart rate of a fetus during labor and delivery are more often the result of a reflex response to changes in the fetus’s circulation than a compression of the umbilical cord or the head. Such drops may also do relatively little or no harm.
Also, scientists today know that cerebral palsy is not caused by a lack of oxygen during delivery in most cases. Instead, birth defects, growth restriction, infections, inflammation and other as-yet unidentified factors cause the condition.
Finally, tests have shown that experienced obstetricians tend to interpret a monitor reading in very different ways. In fact, when an obstetrician was allowed to evaluate the same reading twice several months apart, the interpretation differed even more.
This type of evidence has made the United States Preventive Services Task Force rate electronic fetal monitoring as having the lowest grade of effectiveness possible.
Since electronic monitoring is an inexpensive practice, the lack of benefits would not be an issue if it were not for its association to cesarean sections.
Delivery by cesarean sections have gone hand-in-hand with electronic monitoring, and studies show that a majority of women who deliver in this way first try to deliver vaginally. An electronic reading that is seen as abnormal is partly or entirely the reason most obstetricians decide to switch to surgical delivery.
Clinical trials have also shown that electronic monitoring increases the risk of cesarean sections by 63 percent, and that is without considering that most women who have one surgical delivery will opt out of vaginal birth in the next pregnancy.
Compared to the lack of evidence supporting electronic fetal monitoring, research showing the risks of cesarean deliveries is in agreement.
Bleeding, infections, blood clots blocking vessels, abnormal implants of the placenta in later pregnancies with the risk of catastrophic bleeding, rupture of the uterus, and death are all well-documented consequences for the mother. A study found that death was 3.6 times more common after cesarean sections than vaginal birth. And the newborn child can have difficulties starting breathing.
“It seems intuitively likely that electronic monitoring occasionally enables rescue of a threatened fetus, even if such events are too rare to register in randomized trials or cerebral palsy rates. But is this enough to justify the known harms from increased cesareans?” the team rhetorically asked.
While many people are aware of these facts, there is another force at work driving the development. Obstetricians face a real risk of being held legally responsible for failing to do a cesarean section in time.
Studies show that three out of four obstetricians had at least one professional liability claim, and most had several. The majority of cases also use electronic recordings as evidence in these cases, with plaintiffs’ experts usually being able to show abnormalities in a recording.
But what courts don’t take into account is that examining a reading once the outcome of a child is known is likely to change the interpretation of the reading. And as already mentioned, the prognostic validity of a reading is close to zero.
Nevertheless, a judge without scientific training is likely to take an expert witness at face value, with doctors changing their behavior as a consequence.
To get around this downward spiral, the authors suggest that measures need to be taken. An impartial expert task force taking all available evidence into account would be a first step, they suggested. This process would need to be open to and supported by national and professional healthcare organizations, lawyers, and consumer groups.
Also, to deal with legal claims, a consensus document reviewing the evidence needs to become available to judges to support their assessment of plaintiffs’ experts.
Educating clinicians, lawyers, judges, health policymakers and the public about these factors may help society go back to the practice of intermittent checks in normal-risk deliveries, according to the already present guidelines of birth-related professional societies.


